Procedures
Wisdom Teeth Removal
Thoughtful evaluation and surgical removal of impacted third molars, with comfort-focused care and clear guidance before and after surgery.
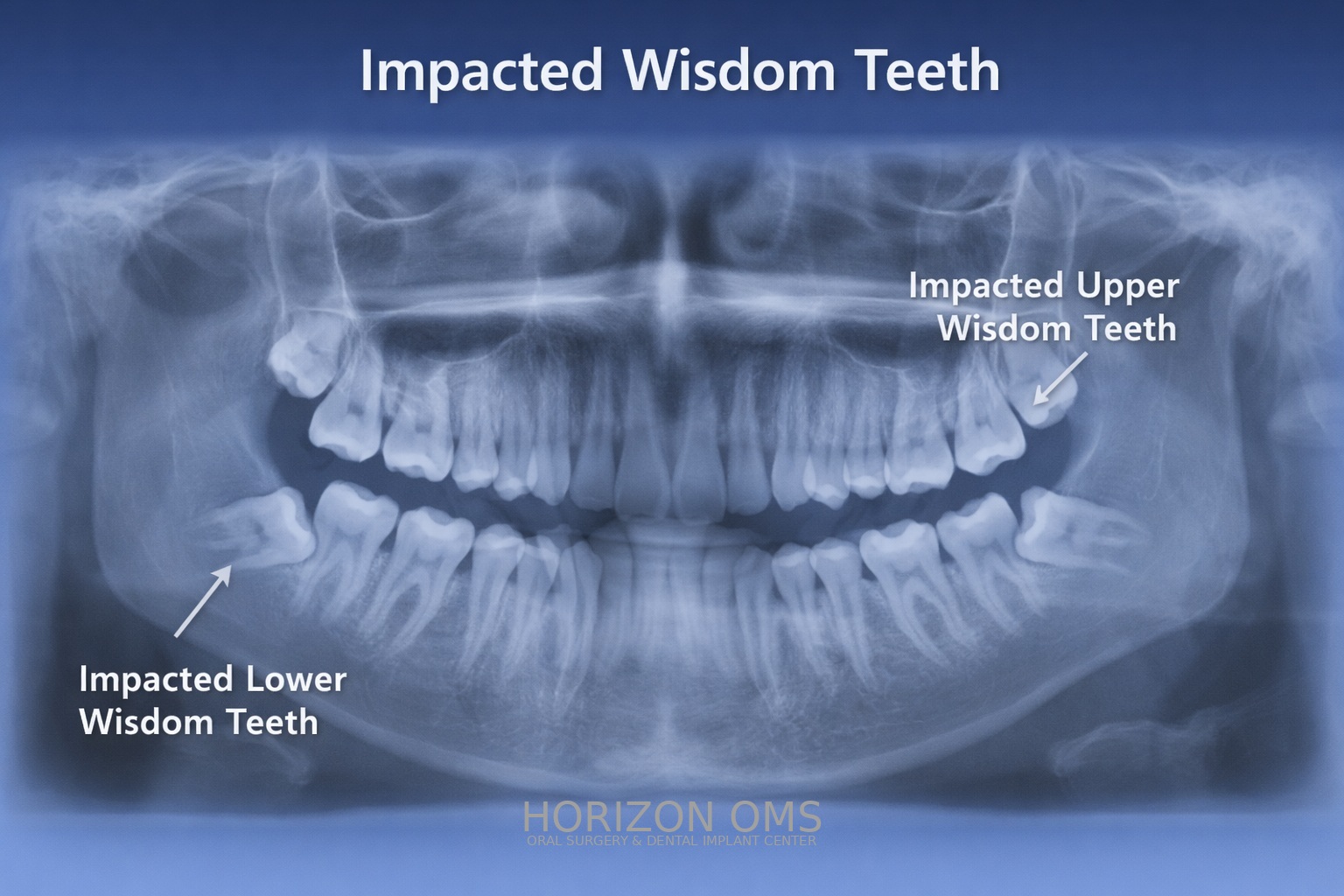
What are wisdom teeth?
Wisdom teeth, also known as third molars, are the last teeth to develop. They often lack adequate space to erupt properly and may become impacted, partially erupted, or misaligned. When this occurs, they can contribute to pain, infection, damage to adjacent teeth, or cyst formation.
When is removal recommended?
- Inadequate space for the tooth to fully erupt — when there isn’t enough room, the tooth can stay partially covered by gum tissue, trap food/bacteria, and become hard to clean.
- Recurrent pain, swelling, or infection
- Impaction or abnormal eruption path
- Risk of damage to adjacent molars
- Associated cysts or pathology
- Orthodontic or surgical treatment planning
What the evidence shows
Even when wisdom teeth don’t hurt, they can still create problems in the area behind the second molars. Because they’re hard to keep clean (especially when partially erupted or angled), bacteria and inflammation can lead to deep gum “pocketing” and bone loss behind the second molars over time — sometimes before you feel symptoms.
Sedation and comfort
Wisdom teeth removal is commonly performed with IV sedation for patient comfort. We review your medical history in advance and discuss sedation options, risks, and expectations on the day of surgery.
Pre‑operative instructions
- Fasting: Do not eat or drink anything for at least 8 hours prior to surgery unless instructed otherwise.
- Medications: Take only medications specifically approved by your surgeon. Bring a current medication list.
- Escort: A responsible adult must accompany you and remain available to drive you home.
- Clothing: Wear comfortable clothing with short sleeves. Avoid jewelry and contact lenses.
- Health changes: Notify our office if you develop illness, fever, or changes in your medical condition.
Why these rules matter: If you’re having IV sedation, fasting lowers the risk of nausea/aspiration, and an escort is required because your coordination and judgment can be affected for the rest of the day.
Post‑operative care
Following surgery, it is normal to experience swelling, discomfort, and limited jaw opening. These symptoms typically improve over several days.
In select cases, bone grafting and/or PRF may be placed at the time of extraction to support healing and reduce complications.
- Bite pressure: Bite gently on gauze for the first 30–60 minutes to control bleeding.
- Swelling: Apply ice packs intermittently for the first 24 hours.
- Medications: Take prescribed medications as directed. Follow your surgeon’s instructions regarding medications.
- Activity: Rest on the day of surgery. Avoid strenuous activity for several days.
Day‑by‑day recovery: what to expect
- Day 0 (surgery day): You’ll be numb at first. Mild oozing is common. Plan to rest, use gauze as directed, and start a soft diet.
- Days 1–3: Swelling and jaw stiffness usually increase and often peak around day 2–3. Bruising can appear. Use ice for the first 24 hours, then switch to warm compresses if recommended.
- Days 4–7: Swelling typically starts to go down and opening improves. Many patients feel well enough to return to normal routines, with a gradual return to regular foods as comfort allows.
- Week 2: Most soreness resolves. The extraction sites continue closing and smoothing out over the next several weeks.
Tip: The risk of “dry socket” is often highest a few days after surgery (commonly days 3–5). Avoid smoking/vaping and straws, and follow your rinsing instructions.
Wound care and oral hygiene
- Avoid rinsing, spitting, or using straws for the first 24 hours.
- After 24 hours, gently rinse with warm salt water after meals.
- Brush teeth carefully, avoiding the surgical sites.
- Avoid smoking or vaping, as this significantly increases the risk of dry socket and delayed healing.
Sedation aftercare
- Do not drive, operate machinery, or make important decisions for 24 hours.
- Have a responsible adult remain with you the evening of surgery.
- Drowsiness, nausea, or dizziness may occur and should improve with rest.
Patient safety note: Even if you feel fine, sedation medications can linger. Having someone stay with you and avoiding driving/decisions helps prevent falls, mistakes with medications, and other avoidable complications.
When to contact our office
Please contact us if you experience excessive bleeding, worsening pain after several days, fever, foul taste or drainage, or any concerns about your recovery.
